What is Keratoconus
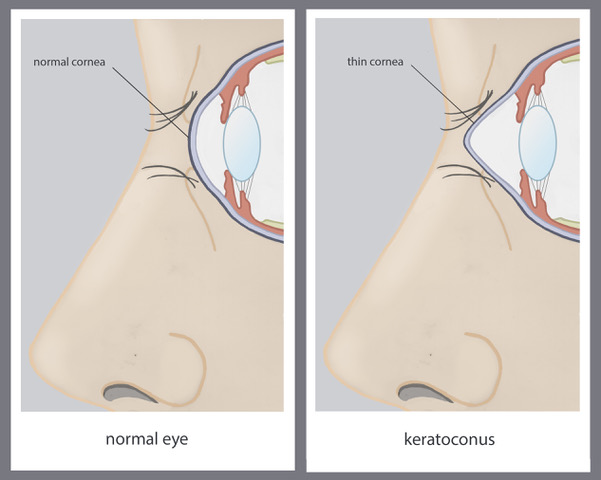
Keratoconus is a degenerative disease of the cornea, in which the cornea progressively thins and a cone-shaped lump is formed. This shape prevents light from focusing directly onto the macula. As the disease progresses, the cone becomes larger and larger, causing blurred and distorted vision.
Because of the irregular shape of the cornea, patients with keratoconus usually have high myopia and high astigmatism, which cannot be corrected with glasses. Keratoconus is often hereditary and usually occurs in both eyes.
Diagnosis & Technology
Early detection is crucial. In our practice we use:
Cornea topography: The most specialized examination that maps the corneal curvature in thousands of points, allowing the detection of the disease even at a subclinical stage.
Pachymetry: To measure the thickness of the cornea and monitor the progression of thinning.
Therapeutic Treatment
Contact lenses: The use of semi-rigid air-permeable (RGP) contact lenses is the basic solution, as they create a new, smooth surface over the irregular cornea.
Cornea transplantation: In advanced stages, where vision cannot be restored with lenses or there is blurring, surgical replacement of the cornea (transplantation) is the final solution.
What are the symptoms?;
Blurred vision that cannot be fully corrected with glasses.
Frequent changes to your glasses prescription.
Photosensitivity and intense “blinding” light at night (halos).
Distorted image of objects.
Frequently Asked Questions
Is keratoconus hereditary?;
Yes, there is a genetic predisposition. If someone in the family has keratoconus, other members (especially in adolescence) should have a preventive corneal topography.
Can I have a Laser Myopia if I have keratoconus?;
NO. Laser myopia (LASIK/PRK) is strictly contraindicated in keratoconus, as the removal of tissue would make the already thin cornea even weaker and dangerous for further deformation.
Why are semi-hard lenses better than soft lenses?;
Soft lenses take the shape of the cornea, so they also carry the deformation of the cornea. Semi-hard lenses keep their shape, creating a perfectly smooth surface in front of the eye, “erasing” the abnormal astigmatism.
Does the progression of keratoconus ever stop?;
Usually the disease progresses until the age of 35-40 years and then tends to stabilize. However, each case is unique and requires regular topographic monitoring.
Does the keratoconus hurt?;
No, keratoconus is painless. If you do experience pain, it may be due to a complication (such as hydrops) or a poor fit of the contact lenses. In any case of pain, contact your doctor immediately.
Should I avoid rubbing my eyes?;
YES. Intense and systematic rubbing of the eyes is considered one of the main factors that aggravate keratoconus. If you have allergies or itching, use special eye drops instead of rubbing your eyes.
